Your Hip Flexors Aren’t Tight, They’re Overworked. Here’s What to Do About It
Today’s guest post comes from Dr. Sarah Duvall, a physical therapist who specializes in women’s health and pelvic function, and who also loves to lift stuff off the floor while helping others do the same. She also has an awesome new course on Postpartum Corrective Exercise Specialist for fitness professionals which is on sale from May 20-th to May 27th 2019, so definitely check it out. She’s updated content and included an entire section on pregnancy considerations to boot. Get it now and save $150!
Hip flexor stretches are all the rage, but if we dig deeper, it sheds some light on why they feel tight and why more stretching might not be the answer. Fixing the cause instead of constantly addressing the symptoms is key for complete postpartum core and pelvic floor recovery, even years down the road.
During pregnancy a woman’s abdominals get stretched out. There is no way to avoid this with a growing baby. Muscles work most effectively when they are at an optimal length. Not too short and not too long. The lengthening that happens during pregnancy puts the abdominal muscles at a decreased advantage for working. This decreases the amount of support they provide for spinal stability.
Since someone has to do the job… (Side note: That’s one of the coolest things about our body. There is always a backup system. Always another set of muscles ready to take over. Even if they are not the most effective and it leads to pain and tightness.) So, who takes over for spinal stability when the abdominals aren’t fully working? The psoas of course.
The psoas is both a primary hip flexor muscle and a core stabilizer because it attaches to the diaphragm, lumbar vertebrae and disc before wrapping around the leg. When we look at full postpartum recovery concerning both the pelvic floor and abdominals (diastasis), we need optimal core functioning, not an overworked psoas.
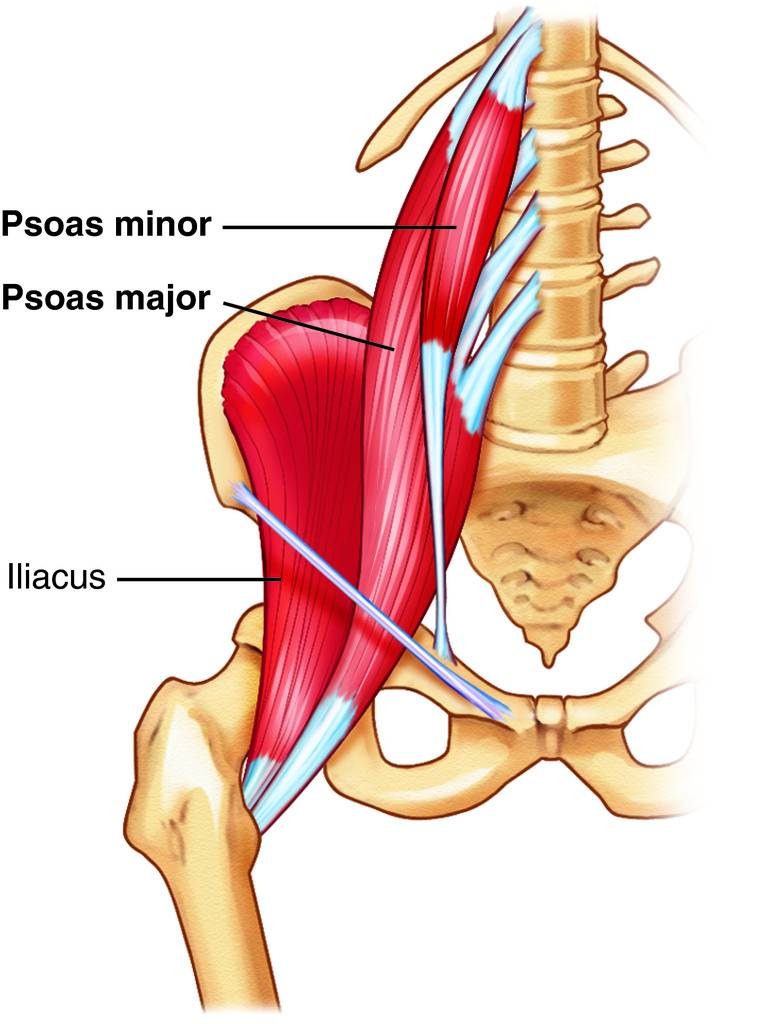
So, why won’t stretching fix the tight psoas in this case? Because we haven’t given anyone else the job of stabilizing the spine. Once you stretch, it just goes right back to being tight because it’s trying to keep your spine safe.
With optimal muscle balance, stretching is highly effective and will hold. That’s why we need to first re-establish function.
Instead of stretching, we need to take pressure off the psoas as a spinal stabilizer so it can work as a primary hip flexor again.
Why does it tighten down so much when overworking as a spinal stabilizer? Remember that length tension relationship we talked about? Well, if the psoas is tight, it can compress the spine easier, thus providing spinal stability. Plus, it has to work a lot to stabilize the spine. When you don’t have correct functioning of the diaphragm and abdominals, the psoas holds a great deal of tension to do the job. This tightness or tension makes it a very ineffective hip flexor.
So, what happens when the psoas is too busy acting as a spinal stabilizer to do it’s job as a hip flexor?
Never fear, your TFL is ready to pick up the slack. Ever foam roll your front pocket? Yikes it hurts! Suffer from Knee pain or IT band tightness or pain? Yep, that’s the TFL and a sign it’s overworking.
Now, both of the primary hip flexor muscles, the psoas and TFL, are tight! All due to an ineffective core stabilizing strategy!
How do we fix this?
Step #1. Decrease back tightness to allow the front to work. If the insertion point of the psoas and diaphragm into the back is tight because it’s overworking for postural control, this will create a pull that the weak, ineffective abdominals cannot overcome. This disrupts the natural front to back balance of core strength.
I’m not talking about doing more sit-ups. That will often create a dominant rectus abdominus that adds more dysfunction to the system. I’m talking about all the abdominals working equally together with the pelvic floor, diaphragm and multifidi.
So, step one is to place the abdominals at an advantageous angle to work by getting rid of this high hinge point, also known as posterior mediastinum tightness.
This will help release the psoas naturally and allow all the core muscles to kick in.
If you’re like me, you’re wondering why our systems don’t “bounce back” or easily recover from having a baby. Aren’t we made to have babies and keep on functioning? Well, evolution hasn’t caught up to modern society yet. When we sit, we hold tension in our hip flexors.
Resting in a full squat helps loosen the psoas by promoting back body diaphragm expansion and putting it in a fully shortened positioned.
Relaxing in a full squat works for releasing the psoas if you’re comfortable. If you’re desperately trying not to fall over backwards, then you’re probably tightening your hip flexors to hold yourself up. This defeats the entire purpose of a resting squat. Grab something like a pillow or a couple books to throw under your heels and see if you can sink down and “rest” into a resting squat. Hold that for a little bit taking some really deep breaths directing the air and pressure of your breath into your back. Then stand up and move around. I bet your hip flexors will feel looser than before the resting squat.
Now, that we have decreased some of the tension in the back, we can focus on strengthening the front. There are loads of awesome core exercises, but let’s take a look at the most common one and make a couple modifications for this postpartum population. Just keep in mind, these are things to look for in a woman that’s 8 weeks or 8 years postpartum. Just because it’s years later doesn’t mean she fully recovered.
Step #2. Rebuild core stability to take the pressure off the psoas.
Now, let’s look closer at what happens in the lower half of the body when the TFL starts taking over for the lack of psoas activity in hip flexion.
The more the TFL has to compensate for the psoas the tighter and more over worked the TFL gets.
The TFL likes to play “King of the Mountain” with the glutes to see who gets to be in charge. You remember that game as a kid? Well, the TFL is pretty good at it and if it’s already overworking to pick up slack from the psoas, it will be even better at winning. Give that muscle an inch and it will take a mile.
As you work through this chain of events down from your diaphragm, you should notice your glutes turn on easier. As the psoas gets to play a bigger role in hip flexion the TFL can let go, and this makes it easier for the glutes to activate. Who doesn’t love glutes?
You should start to feel more glute participation during all of your exercises, including walking and running. Creating balance in your core can be the difference between getting stronger safely and a line of injuries, like back pain, knee pain or pelvic floor issues.
Let’s wrap this up with a recap on breathing.
Without back body expansion during each breath we continue to perpetuate the tight hip flexor scenario. This is often accompanied by decreased pelvic floor recovery since the pelvic floor works in synch with the diaphragm. These women will often be dealing with sneeze pee, leaking with jumping or prolapse. Without awesome diaphragm expansion, we can’t have a great pelvic floor. They are too intertwined in their functioning.
The same lack of correct breathing also perpetuates a diastasis. Without proper deep breathing, you can compensate a couple ways. The first is to draw in your belly button and go into a shallow breathing pattern and the second is to have belly only expansion. Both of these can hinder diastasis healing. The cool thing is that I’ve actually had women experience spontaneous firming of their diastasis when we get down a correct breathing pattern. It’s a phenomena that always amazes me. The same thing can happen with decreasing prolapse symptoms.
To cap it off, here are a couple common breathing mistakes I see frequently.
Want to learn more about full postpartum recovery, including diastasis and all pelvic floor issues? Check out her PostPartum Corrective Exercise Specialist course while it’s on sale until May 27th 2019.

7 Responses to Your Hip Flexors Aren’t Tight, They’re Overworked. Here’s What to Do About It